Learn About DVT - Deep Vein Thrombosis
Deep vein thrombosis (DVT) is the formation of a blood clot (thrombus) within a deep vein.
It commonly occurs in the thigh or
calf. Deep vein thrombosis can develop after any major
surgery. People who have surgery on the legs and hip are especially at risk.
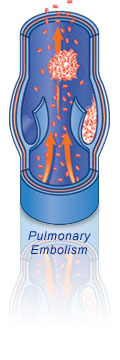
A pulmonary embolism (PE) is a clot that breaks free and travels through the veins.
If it reaches the lungs, it can block the
flow of blood to the lungs and heart. A pulmonary embolism is a dangerous condition that can even lead to death.
- Blood that flows slowly through veins (stasis). The walls of veins are smooth. This helps blood flow and mix with naturally occurring agents (anticoagulants) that keep blood from clotting. Blood that does not flow and does not mix with anticoagulants may lead to blood clots. This is why it is important to watch for signs of DVT in people who are in bed, or do not move, for long periods of time.
- Coagulation. Blood thickens (coagulates) around matter that does not belong in the veins. During surgery, matter like tissue debris, collagen, or fats can be released into the blood system.
- Damage to the vein walls during surgery. A surgeon must move (retract) tissues, such as muscle, ligaments, and tendons, to reach the area being operated on. Sometimes, this can release naturally occurring substances that promote blood clotting.
- Other factors. These include age, previous history of deep vein thrombosis or pulmonary embolism, cancer, vein disease (such as varicose veins), smoking, estrogen usage or current pregnancy, obesity, and genetic factors.
Find more details relating to causes of DVT at aaos.org
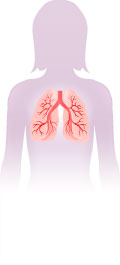 Deep vein thrombus is a clot that can form in the leg and
move to your lungs. Classic signs of a DVT include calf discomfort, edema, distended veins, or foot pain. But, fewer than a third of patients with DVT show these signs.
Deep vein thrombus is a clot that can form in the leg and
move to your lungs. Classic signs of a DVT include calf discomfort, edema, distended veins, or foot pain. But, fewer than a third of patients with DVT show these signs.
After hip surgery, clots (thrombi) often form in the veins of the thigh. These clots are more likely to lead to a pulmonary embolism. After knee surgery, most thrombi occur in the calf. Although less likely to lead to pulmonary embolism, these clots are more difficult to detect.
Find more details relating to signs & symptoms at aaos.org
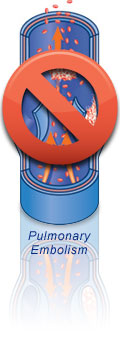 Both DVT and PE may be asymptomatic and difficult
to detect. Thus, physicians focus on preventing their development by using mechanical or drug therapies. Without this preventive treatment, as many as 80% of orthopaedic
surgical patients would develop deep vein thrombosis, and 10% to 20% would develop pulmonary embolism. Even with these preventative therapies, DVT and subsequent
PE remain the most common cause for emergency readmission and death following joint replacement.
Both DVT and PE may be asymptomatic and difficult
to detect. Thus, physicians focus on preventing their development by using mechanical or drug therapies. Without this preventive treatment, as many as 80% of orthopaedic
surgical patients would develop deep vein thrombosis, and 10% to 20% would develop pulmonary embolism. Even with these preventative therapies, DVT and subsequent
PE remain the most common cause for emergency readmission and death following joint replacement.
Prevention is a three-pronged approach designed to address the issues of stasis and coagulation. Usually, several therapies are used in combination. For example, a patient may be fitted with graded compression elastic stockings and an external compression device upon admittance to the hospital; movement and rehabilitation begin the first day after surgery and continue for several months; anticoagulant therapy may begin the night before surgery and continue after the patient is discharged.
TIP: Download the checklists in the left column for a handy reference on DVT prevention at home or while traveling.
Find more details relating to prevention at aaos.org
Links to other websites and content are provided for informational purposes only. Such links in no manner indicate Panhandle Orthopaedics' endorsement,
recommendation, affiliation, or relationship with the owners of such linked websites or the services or goods presented in such linked websites unless otherwise noted. Panhandle Orthopaedics
has no control over or responsibility for the content or availability of any linked websites or the services or goods presented in such websites.
This site does not provide medical advice. Please review the full Medical Disclaimer before using this resource.


